A new treatment for Parkinson’s disease could be on the horizon after scientists used an ultra-powerful scanner to study a secluded part of the brain. The machine, capable of scanning a grain of sand in great detail, will also help identify who would benefit from the new drugs, while clinical trials are already underway, according to a new study.
It’s estimated that nearly 1 million people in the U.S. are living with Parkinson’s disease, according to the Parkinson’s Foundation. Approximately 60,000 new cases are recorded each year. About three out of every 100,000 people in the U.S. are diagnoses with a related disorder known as progressive supranuclear palsy (PSP).
Drugs like L-DOPA are often prescribed to treat patients with these conditions, as they can help lessen the tremors and shakes. But they do little for non-motor symptoms like the damage caused to a person’s motivation and mental abilities.
Scientists have therefore turned to another chemical dubbed noradrenaline, which is known to play an important role in brain functions, including attention, arousal, thinking and motivation.
“Noradrenaline is very important for brain function,” says lead study author Professor James Rowe, from the Department of Clinical Neurosciences at the University of Cambridge, in a statement. “All of our brain’s supply comes from a tiny region at the back of the brain called the locus coeruleus – which means ‘the blue spot’. It’s a bit like two short sticks of spaghetti half an inch long – it’s thin, it’s small, and it’s tucked away at the very base of the brain in the brain stem.”
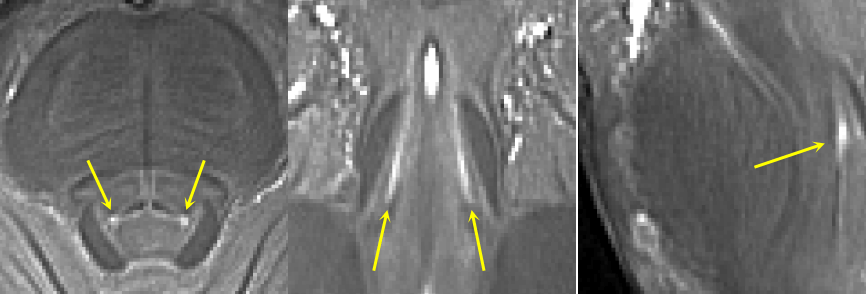
The researchers had examined brains donated to the Cambridge Brain Bank and found some people with PSP had lost 90 per cent of their noradrenaline supply. Studying the locus coeruleus has however proven difficult because conventional MRI scanners do not have a high enough resolution.
“The locus coeruleus is a devil to see on a normal scanner. Even good hospital scanners just can’t see it very well,” says Rowe. “And if you can’t measure it, you can’t work out how two people differ – who’s got more, who’s got less? We’ve wanted MRI scanners to be good enough to do this for some time.”
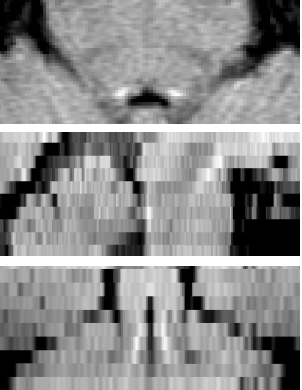
They therefore decided to use a 7T MRI scanner at Addenbrooke’s Hospital in Cambridge which have ultra-strong magnetic fields. While most scanners can see objects the size of a grain of rice in great detail, 7T scanners can go down to a grain of sand.
They used the super scanner to measure changes in the brains of people with Parkinson’s disease, PSP, or who were in good health. People who had sustained more damage to their brain experienced more severe symptoms and scored lower on mental tests, the researchers found.
A number of drugs that boost noradrenaline have already been through clinical trials for other conditions. New treatments for the non-motor symptoms of Parkinson’s disease and PSP could therefore be around the corner.
The researchers have already started clinical trials to see whether these drugs alleviate symptoms in PSP.
“Not every PSP or Parkinson’s patient is going to benefit from noradrenaline-boosting drugs,” says study co-author Dr. Rong Ye. “They’re more likely to benefit those people with damage to their locus coeruleus – and the greater the damage, the more benefit they’re likely to see.”
A 7T MRI scanner will help doctors identify which patients stand to benefit from taking noradrenaline boosting meds.
“This will be important for the success of the clinical trial, and, if the drugs are effective, will mean we know which patients to give the treatment to,” adds Ye. “In the long term, this will prove more cost-effective than giving noradrenaline boosters to patients who ultimately would see no benefit.”
The findings are published in the journal Movement Disorders.
Report by South West News Service writer Tom Campbell