It is estimated that in 2019, 19.4 million Americans had a major depressive disorder — about 7.8 percent of the population. The number was even higher in 2020. It is estimated that 21 million adults in the United States have experienced at least one major depressive episode in their lives. Such high morbidity and mortality call for action. To that call, three institutions — the University of California – San Diego School of Medicine, Weill Cornell Medicine, and Stanford Medicine — are collaborating in an intensive 3-year investigation of methods to prevent or treat major depression.
This collaboration also aims to accelerate treatment responses, and to create methods for developing personalized therapeutic strategies for depression patients.
“Depression is not a singular condition, and there is no singular remedy,” says Dr. Zafiris “Jeff” Daskalakis, chair of the Department of Psychiatry at the UCSD School of Medicine, in a statement. “It is an extraordinarily complex disease that, in many ways, is not well-understood. It is a different disease in every person.”
Daskalakis co-leads the program with Dr. Conor Liston, associate professor of psychiatry at Weill Cornell, and Dr. Nolan Williams, assistant professor of psychiatry and behavioral sciences at Stanford Medicine
Depression is usually treated with psychotherapy and/or drugs that target defined functions, such as selective serotonin reuptake inhibitors (SSRIs). These approaches are effective for many patients, but about one-third of patients derive no benefit from drugs.
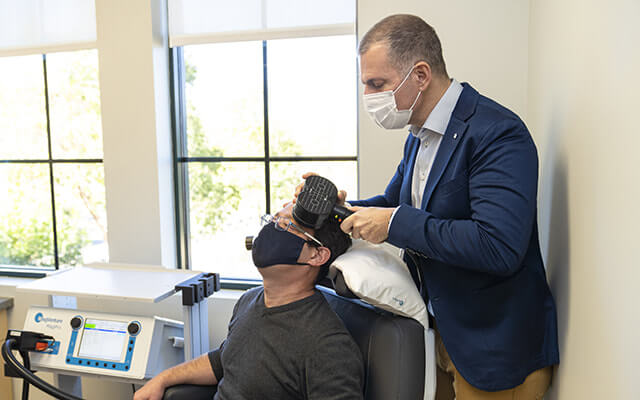
Liston, Williams, Daskalakis and colleagues will focus on current and new uses of transcranial magnetic stimulation (TMS), in which series of short magnetic pulses stimulate nerve cells in areas of the brain known to be associated with major depression. UC-San Diego Health was the first provider of TMS for individuals with treatment-resistant depression.
“TMS requires patients to come to the clinic daily, and medications do not,” says Liston. “So, for many people, medications are a good first treatment to try, but TMS is a great option for people who do not respond to medications.”
During the three-year study, participants will receive various treatments, including a combination of an antidepressant and different types of TMS.
Patients will be evaluated through clinical assessments and brain scans. The premier goal is the development of algorithms that match individuals with personalized treatment plans for their depression.