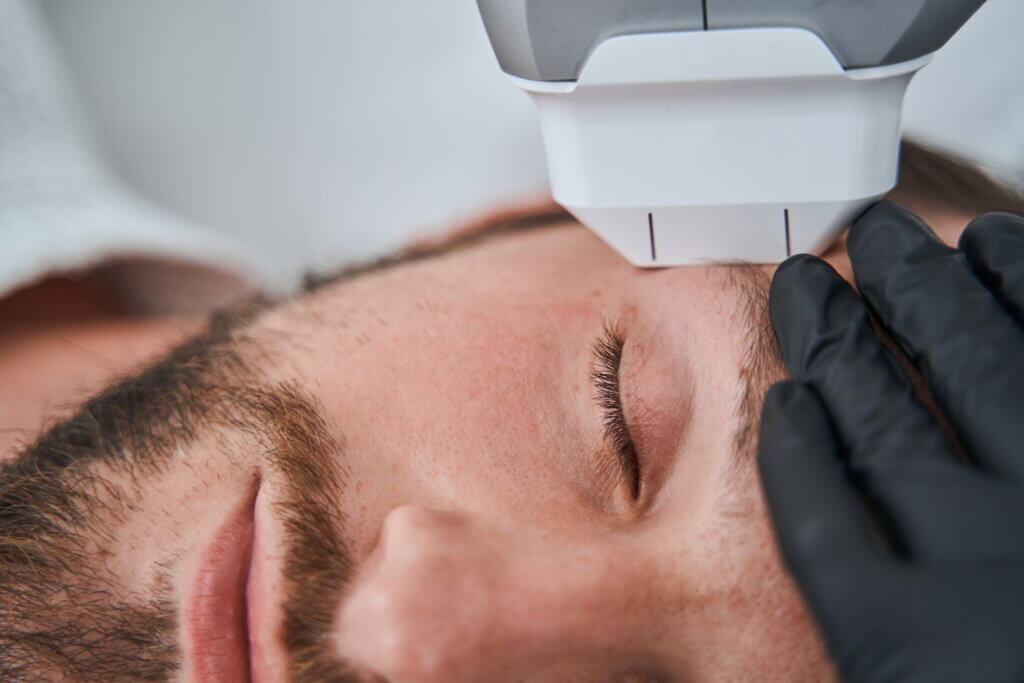
That familiar ache of a headache or stiff joints has most of us automatically reaching for the ibuprofen bottle. But what if instead of popping a pill, you could simply manipulate a spot deep in your brain to switch off pain? New research shows that focused pulses of ultrasound aimed precisely at the insula—the region of the brain associated with pain perception—can significantly reduce feelings of pain as well as the body’s physical responses to it.
The proof-of-concept study, led by Wynn Legon, an assistant professor at the Fralin Biomedical Research Institute at Virginia Tech, marks the first time focused ultrasound has been used to target the insula. And the team’s results, published this month in the journal PAIN, demonstrate that this noninvasive approach can lessen both the subjective sensation of pain and objective measures like heart rate.
“Can we get the focused ultrasound energy to that part of the brain, and does it do anything?” Legon asked in a media release. “Does it change the body’s reaction to a painful stimulus to reduce your perception of pain?”
So how did the researchers zap pain away with sound waves? Let’s break it down.
Feel the Heat, Feel the Pain
The study involved 23 healthy volunteers who received mild heat stimulation on their hands meant to cause pain. At the same time, the participants wore a device that used MRI imaging to guide sound waves precisely to the anterior insula—a region buried deep in the brain that plays a key role in pain perception and regulation.
Throughout the experiments, the participants rated their pain levels on a scale from 1 to 10. Researchers also monitored their heart rate and heart rate variability (small fluctuations between heartbeats) to gauge how ultrasound stimulation of the insula affected the body’s physiological response to pain.
Turning Down Pain Dials in the Brain
So did beaming sound waves into the brain actually ease the participants’ pain? Yes, according to the results: on average, they reported a 0.75 point drop in pain levels when the ultrasound was switched on compared to when it was off.
“That might seem like a small amount, but once you get to a full point, it verges on being clinically meaningful,” Legon explained. “It could make a significant difference in quality of life, or being able to manage chronic pain with over-the-counter medicines instead of prescription opioids.”
In other words, while a 0.75 point change might not seem huge, even subtle reductions could have an outsized impact on those dealing with chronic, debilitating pain. What’s more, dampening pain signals in the brain appeared to calm the body too: heart rate and heart rate variability measures indicated reduced physiological stress when the ultrasound device was active.
“Increasing the body’s ability to deal with and respond to pain may be an important means of reducing disease burden,” said Legon.
Soundwave Surgery Without the Surgery
So how exactly can pulses of ultrasound energy act like a mute button for pain? The technology actually builds on advances in ultrasound imaging used to visualize developing babies during pregnancy. But instead of scanning tissues, low-intensity focused ultrasound (FUS) delivers targeted energy to precise spots deep in the body—in this case, critical neural circuits in the insula.
“At high intensity, ultrasound can ablate tissue. At low intensities, it can cause gentler, transient biological effects, such as altering nerve cell electrical activity,” the researchers note in the media release.
Previous research has explored using electromagnetic stimulation to modify brain activity for treating conditions like depression. But Legon’s study is the first to demonstrate that focused ultrasound can safely access and modify deep brain regions that play key roles in our perception of pain.
Insula and Interoception: The Brain’s Pain Center
But why specifically target the insula? Scientists have learned this region essentially serves as headquarters for the brain’s master pain map. Specifically, the anterior insula plays a key role in interoception—our awareness of internal body sensations like pain, hunger, body temperature, and other visceral feelings.
The anterior insula is basically reading all of this information constantly streaming from the body below the level of consciousness. When there’s something that requires attention, that seems to be painful or threatening, then it gets pulled up into consciousness.
This role as mission control for physical and emotional awareness helps explain why stimulating the insula could change pain perception: dial down activity in this critical hub, and the sensation of pain likely diminishes too.
Future Directions: Exploring the Heart-Brain Connection
While decreases in pain score and stress hormone levels are promising, Legon emphasizes this is just the first glimpse of focused ultrasound’s potential for noninvasive neuromodulation. There are no shortage of ideas to explore next, including investigating whether tweaking brain activity could help disorders involving the heart-brain connection.
“Your heart is not a metronome—the time between your heartbeats is irregular, and that’s a good thing,” said Legon. “The effect of focused ultrasound on those factors suggests a future direction for our research.”
Specifically, scientists want to explore what’s known as the heart-brain axis: how the heart and brain signal each other, and whether mitigating pain’s cardiovascular effects could lessen its burden. Considering the opioid epidemic’s tragic outcomes, developing alternative chronic pain treatments remains critically urgent.
In the meantime, focused ultrasound procedure could be a true game-changer for chronic pain. Larger and longer clinical studies will be needed to evaluate real-world efficacy. Such technologies could one day provide chronic pain relief without pills’ risk of side effects and addiction—offering new hope to those feeling more than their fair share of pain.