Patients with deadly brain tumors could potentially be cured by a new drug. The breakthrough therapy switches off genes that fuel tumors known as glioblastomas (GBMs).
Scientists from the U.S. and United Kingdom are planning a clinical trial on the glioblastoma drug after successful experiments on mice and cells grown in the lab. The international team created a cocktail of chemicals that target what’s known as “Hox” genes.
Fewer than half of sufferers survive beyond a year of being diagnosed with a glioblastoma. President Joe Biden’s son Beau died from the disease in 2015.
“People who suffer from glioblastomas have a five percent survival rate over a five-year period – a figure that has not improved in decades,” says project leader Hardev Pandha, a professor of medical oncology the University of Surrey, in a statement. “While we are still early in the process, our seven-year project offers a glimmer of hope for finding a solution to Hox gene dysregulation, which is associated with the growth of GBM and other cancers, and which has proven to be elusive as a target for so many years.”
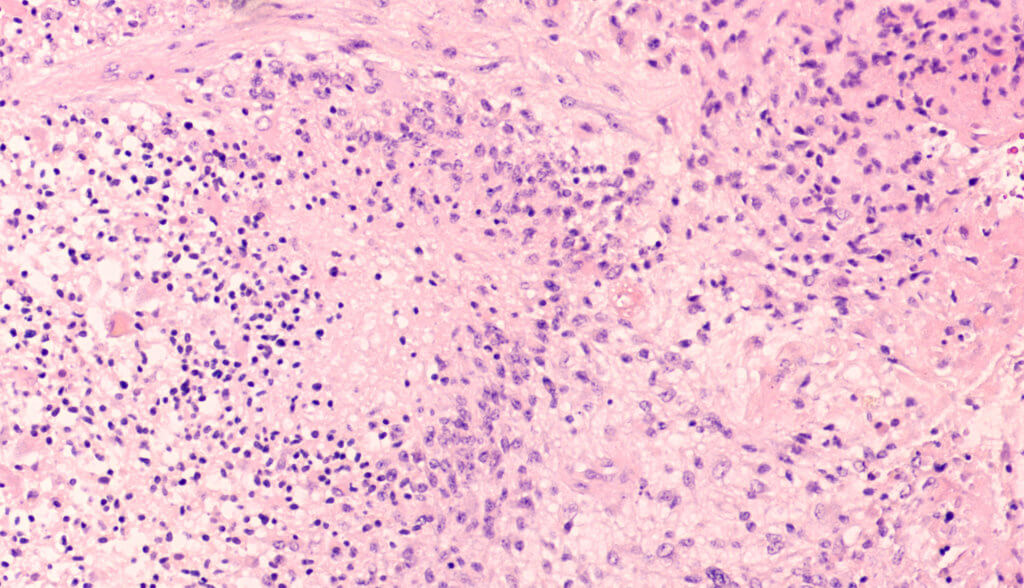
The peptide, named HTL-001, contains short chain amino acids, the building blocks of proteins. Ironically, Hox genes are responsible for the healthy growth of brain tissue. They are ordinarily silenced at birth after vigorous activity in the embryo. If they are inappropriately “turned on” again, it can lead to the progression of cancer. Hox gene dysregulation has long been recognized in GBM.
Brain tumors are rare. Glioblastomas affect an estimated one in 30,000 people. They
develop when cells supporting nerves in the brain begin to divide uncontrollably. Surgery is the main treatment. About 40 percent of patients survive beyond a year, and just 17 percent more than two years.
“We desperately need new treatment avenues for these aggressive brain tumors,” says co-author Susan Short, a professor at the University of Leeds. “Targeting developmental genes like the HOX genes that are abnormally switched on in the tumor cells could be a novel and effective way to stop glioblastomas growing and becoming life threatening.”
Hox genes have been linked to a host of common cancers ranging from colon, breast, ovarian and cervical to leukemia. The HTL-001 peptide is suitable for patient trials after passing safety tests, say the researchers. They are now being considered for glioblastomas and other cancers.
James Culverwell, CEO of University of Surrey start up HOX Therapeutics, says the breakthrough reported in BMC Cancer is exciting. “We hope with our continuing support, this research will eventually lead to novel and effective treatments for both brain and other cancers where HOX gene over-expression is a clear therapeutic target,” he adds.
The study is published in the journal BMC Cancer.
Report by South West News Service writer Mark Waghorn.










NWBO – tomorrow
This is great news, but too late for an old friend who died from brain cancer a while back.
Shortly after his Dx, we were talking about life, our hopes, ambitions, etc. His only ambition was to stay alive long enough for them to find a cure. Sadly he lost the race – and his wife did too a year later.
You could treat patients with an antisense molecule directed toward the HOX gene. I once treated glioblastoma using antisense against EGFR, another gene active in glio.
Let’s hope this happens sooner rather than later. It’s great to read about potential breakthroughs but then it all goes quiet. I am 15 months since initial diagnosis so getting close to the terrible prognosis dates! And have a recurrence at the moment so any breakthrough in treatment can’t come soon enough.