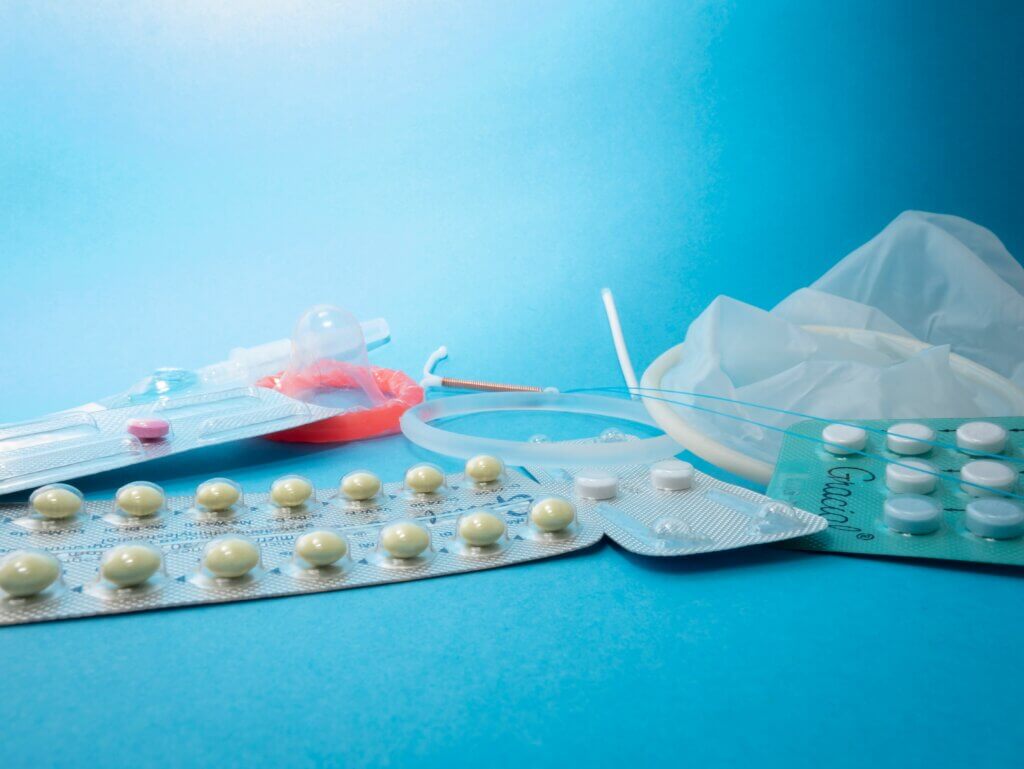
Progestogens, a class of hormones commonly used in birth control pills and menopausal hormone therapy, have long been a mainstay of women’s health treatments. But a new French study, published in the journal The BMJ, warns that some of these widely prescribed drugs may come with a serious hidden risk: a heightened chance of developing meningioma, the most common type of brain tumor.
Researchers from the French National Agency for Medicines and Health Products Safety and French National Health Insurance analyzed health records from over 100,000 French women, tracking their progestogen use and meningioma diagnoses over a 10-year period. They discovered that prolonged use of certain progestogens — namely medrogestone, medroxyprogesterone acetate, and promegestone — was associated with a significantly increased risk of these typically benign but potentially disabling brain tumors.
Meningiomas, which form in the protective membranes surrounding the brain and spinal cord, are usually slow-growing. But as they get bigger, they can compress nearby brain tissue, causing symptoms like headaches, vision and hearing problems, seizures, and even personality changes. In serious cases, surgery to remove the tumor is necessary.
That’s why the study’s findings are so concerning: women who took the implicated progestogens for a year or more were several times more likely to require meningioma surgery compared to non-users. And while meningiomas are more common in older adults, some progestogen-related cases were seen in women as young as 35.
Progestogens mimic the effects of progesterone, a natural hormone involved in the menstrual cycle and pregnancy. Previous research has shown that over 60 percent of meningiomas have progesterone receptors on their surface. Theoretically, progestogens could stimulate these receptors, promoting tumor development and growth.
The risk seems to vary between different progestogens. While medrogestone, an oral medication used for menopause and menstrual disorders, was associated with a 3.5-fold risk increase, the injectable contraceptive medroxyprogesterone acetate (Depo-Provera) carried a whopping 5.5-fold higher risk. Promegestone, another oral progestogen, had a 2.4-fold increased risk.
In contrast, several other progestogens showed no significant link to tumor risk, including natural progesterone, a similar oral medication called dydrogesterone, and the levonorgestrel intrauterine system (hormonal IUD). This suggests that not all progestogens affect the brain equally and that more “natural” formulations may be safer.
Researchers estimate that up to 0.5 percent of meningioma surgeries in France could be attributed to the use of the implicated progestogens. While that may sound small, it translates to dozens of potentially avoidable brain surgeries each year. And in countries where medroxyprogesterone injections are a more popular form of birth control, like many lower-income nations, the impact could be even greater.
There are some key limitations, researchers state. The study relies on medical records, which don’t provide details on exactly why each woman was prescribed progestogens. Certain conditions that warrant progestogen treatment, like endometriosis or heavy menstrual bleeding, might themselves influence meningioma risk. The records also didn’t specify tumor size or symptoms, so some women may have had small meningiomas that didn’t require treatment.

Still, the results raise serious questions about the safety of certain progestogens, especially with long-term use. While these medications can offer important benefits like contraception and menopausal symptom relief, the potential brain tumor risk can’t be ignored. Researchers call for further research into dose-response relationships and tumor characteristics to better understand the progestogen-meningioma link.
In the meantime, women and their doctors should carefully weigh the pros and cons when considering progestogen therapy, particularly if using it for an extended period. Opting for lower-risk formulations like progesterone or dydrogesterone may be a smart strategy. And anyone experiencing possible meningioma symptoms should promptly seek medical evaluation.